A general dentist orthodontic course can teach you how inflammation plays an important role in your patients’ orthodontic journey.
Orthodontics is not just about moving teeth to create a perfect smile. Orthodontic treatment can form a balanced bite, correct TMJ problems, and improve a person’s quality of life. While braces may look straightforward, dentists know there is extensive physics and biology that is correlated with orthodontic treatment, and it takes knowledge and training to be able to create those straight, beautiful smiles.
What is orthodontics?
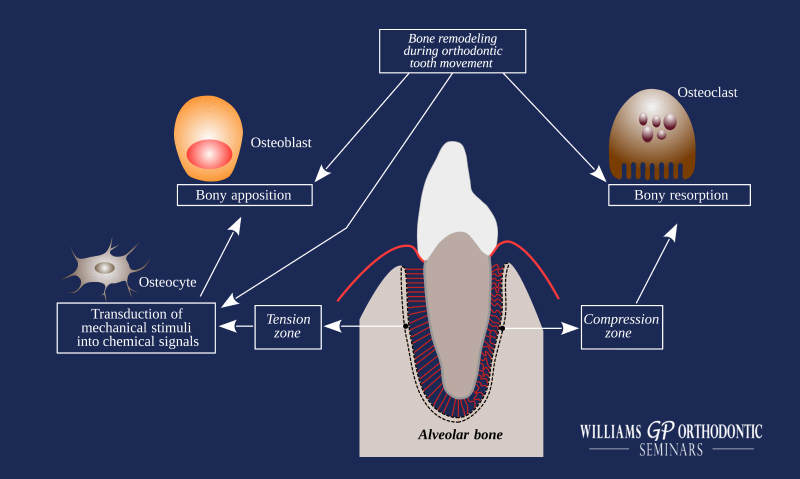
Orthodontics is the movement of the entire tooth (including the clinical crown and root) by remodeling of the alveolar bone and periodontal ligament (PDL). Tooth movement is a complex and intricate process that relies on cellular mechanisms of the breakdown of bone and deposition of bone. Orthodontic forces from brackets and wires help teeth to move by putting a tension and force on the PDL to signal an immune response.
How does inflammation play a role in orthodontics?
Just like inflammation can play a role in our bodies during illness, it also plays an important role in orthodontics, and without it, teeth would not be able to move into their correct position and be retained stably.
When forces are applied in orthodontics to shift teeth into the proper position, there are biomarkers that are present on a microscopic level that indicate the healthy physiologic process, but can also indicate if there is any iatrogenic pathology causing bone resorption and pathologic inflammation.
Dentists trained to treat orthodontic patients understand that specific forces are necessary to stimulate an immune response. This immune response indicates a cellular change in the bone, neural change, vascular change, and a PDL change.
In healthy tooth movement, there are harmonious tension and compression sites caused by orthodontic forces that result in these immune responses and tissue changes. Understanding orthodontics means understanding the proper use of heavy versus light forces, and continuous versus intermittent forces to allow for a healthy immune response.
On a cellular level, there are different biomarkers observed depending on the time frame of orthodontic tooth movement.
- Initial movement phase (two days): An acute inflammatory process is observed that signals bone to remodel. This occurs when the tooth first moves in the socket.
- Arrest phase (20 to 30 days): Movement stops, but there is chronic inflammation observed with paradental bone remodeling.
- Acceleration phase (40 days): Following initial tooth movement, there is another period of acute inflammation overlapping with chronic inflammation.
- Linear phase: At this phase, there is actual tooth movement and there is a microcellular observance of osteoblasts, osteoclasts, and alkaline phosphatase activity.
How do dentists know when there is bone breakdown and bone remodeling? When there is an inflammatory process, inflammatory mediators are released in the gingival crevicular fluid.
Mediators that signal there is bone resorption include:
- Prostaglandin E-2.
- Substance P.
- Epidermal Growth Factor.
Bone remodeling markers observed in gingival crevicular fluid includes:
- Transforming Growth Factor.
- Interleukin 1β,2,6,8.
Can the inflammatory process be positive and negative in tooth movement?
Tooth movement requires the disturbance of the PDL and alveolar bone, but ideally, only the lightest forces in orthodontics are recommended. This is because when slow, light forces are applied to teeth, the alveolar bone breaks down in response to inflammatory markers, and at the same time there is bone remodeling for stable results.
When heavy or quick orthodontic forces are applied, there is greater risk for an inflammatory process that is detrimental to the alveolar bone, PDL, and roots of teeth. This may result in bone breakdown without remodeling and can cause severe root resorption.
In order to prevent root resorption and potential tooth loss, general dentists who practice orthodontics attempt to slow down treatment time. Studies show that heavy forces, while accelerating tooth movement, results in necrosis of bone and can cause tooth mobility and tooth loss.
How can you learn more about orthodontic tooth movement?
Orthodontics is not a topic that can be learned in a single continuing education class. It is a comprehensive dental topic that requires much knowledge, training, skills, and confidence. This is one of the top reasons Dr. Brad Williams offers an orthodontic continuing education course for general dentists that spans several months in five sessions. Each session contains two days of didactics and a hands-on learning component to understand real-life treatment plans.
The role of inflammation is important for dentists to understand so they can avoid performing iatrogenic treatment and causing poor long-term results. There is a delicate balance between trying to accelerate tooth movement and allowing for the body to reabsorb and remodel bone in the healthiest way. In our Basic Straight Wire Course, we go the extra mile to provide a solid knowledge base as well as hands-on experience so you can implement orthodontics with competence and confidence.
Taking a general dentist orthodontic course is the first step to get a solid foundation in the biology and biomechanics of orthodontics. Once you understand the physics of tooth movement, the technical skills will easily follow, and you will be able to provide high quality dental care for your patients. If you’re interested in learning more about orthodontics and the biologic forces behind tooth movement, contact Williams GP Orthodontic Seminars to enquire about our upcoming courses.